Patients with blood disorders to get world-first NHS test
Sickle cell patient gets world-first NHS test
A patient with sickle cell disorder says she is optimistic for the future after a new genetic test was launched.
Stephanie George, 32, from London, was one of the first patients to receive a "blood matching" genetic test at Whittington Hospital in north London.
The genotyping test aims to better match patients' blood transfusions and reduce the risk of side effects.
On Monday, the NHS became the first healthcare system in the world to provide the blood group test.
It means almost 18,000 patients living with sickle cell disorder and thalassaemia in England are now eligible for more accurate blood matching.
Ms George said: "Sickle cell affects my life every day.
"We're not lazy, we have a blood condition and yes it is debilitating but we still want to live as normal a life as we possibly can."
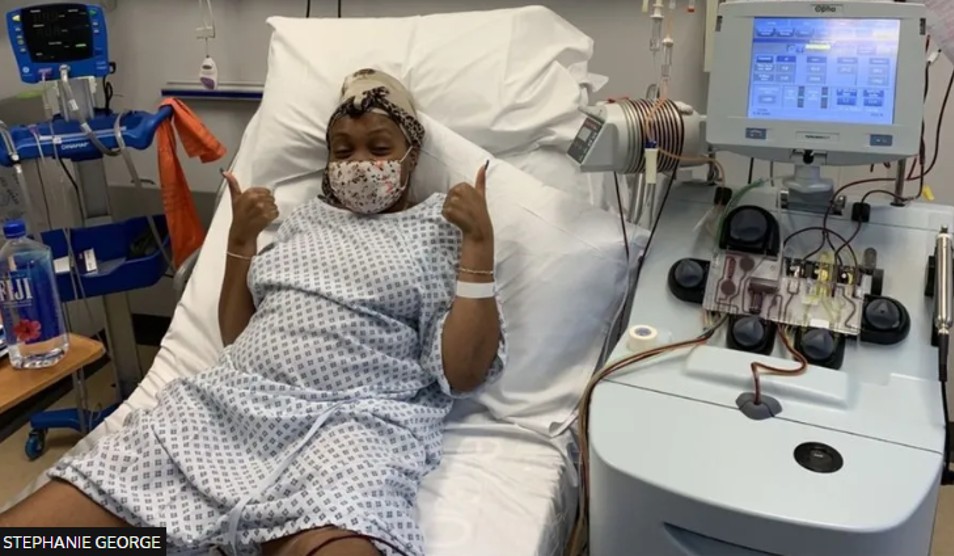
'Patients need it'
She has been having blood transfusions for more than 20 years, and receives them around every six weeks.
"I do think the new test will be really great," she said. "This illness has been around for such a long time and I'm glad the technology is starting to catch up, because patients need it."
A world-first NHS test which could help reduce the risk of side effects from blood transfusions are being offered to thousands of patients with inherited blood disorders.
It is the first healthcare system in the world to provide the new test, which some 18,000 people in England are eligible for.
From Monday, people with sickle cell disorder and thalassaemia in England will have access to a genetic test to better match their blood transfusions and offer more personalised care.
Professor Bola Owolabi, director of the National Healthcare Inequalities Improvement Programme at NHS England, said: “This world-first test is yet another example of the NHS leading the way to transform care and improve outcomes and quality of life for thousands of patients with sickle cell disorder and thalassaemia.
“Being able to provide high-quality and more personalised care to people with inherited blood disorders is an important step forward in helping to reduce health inequalities and this innovative test will greatly improve quality of life for people living with these disorders.
“I urge those eligible to ask their clinical teams about the test and to accept if they are invited to take part.”
Life-saving transfusions are commonly used to treat rare inherited blood disorders, but after transfusion, around a fifth of patients develop antibodies against certain blood groups.
They can then experience delays to treatment due to the difficulty in finding enough matching blood and sometimes blood transfusion reactions.
DNA analysis of a patient’s blood group may help find the best compatible blood for patients with complex requirements, with some donor blood being tested in a parallel programme.
To help improve blood-matching and reduce the risk of antibodies developing, NHS England, in partnership with NHS Blood and Transplant (NHSBT), is encouraging patients with sickle cell, thalassaemia and transfusion-dependent rare inherited anaemias to have this test alongside their routine hospital blood tests.
The condition, which is more common in people of black African and Caribbean heritage, can result in severe organ damage and intense pain if damaged red blood cells block vessels and restrict oxygen supply.
People with thalassaemia cannot produce enough haemoglobin, which is used by red blood cells to carry oxygen around the body, causing severe anaemia – which can be fatal if not treated.
Thalassaemia is mainly seen in those with an Asian, Middle Eastern, Southern Mediterranean heritage, with about 800 patients in England and less than 50 new cases each year.
The new test will also help patients living with transfusion-dependent rare inherited anaemias, such as Diamond Blackfan Anaemia, a disorder that affects people’s production of red blood cells.
John James, chief executive of the Sickle Cell Society, said: “With the introduction of this innovative test, we take a remarkable stride towards achieving better blood matches for all those living with the condition.
“We urge individuals with sickle cell disorder to have the blood test as it will not only support more accurate treatment but also hold the potential to save more lives in the future.”



